Informatics - Electronic Health Record Life Cycle
Informatics - Electronic Health Record Life Cycle
Course Description
This course discusses the EHR Life Cycle model and includes content regarding hardware and software requirements, planning, execution, management, measuring effectiveness, and quality assurance.
Accreditation Information: KLA Education Services LLC is accredited by the State of California Board of Registered Nursing, Provider # CEP16145.
Course Certification: Once you have completed this course, click on the “Print Certificate” option below to save or print your CE course certification. If you are not yet registered in a course plan with IvyLeagueNurse, please complete the registration and payment process so that you are able to log into your account and fully obtain your course certificate. Our affordable and unlimited one-year CEU plan starts at just $19.99.
Print Certificate Print Course
Course Objectives
Upon completion of this course, the course participant will be able to:
- List the 4 phases of the EMR life cycle
- Discuss and example Need.
- Discuss an example Solution.
- Discuss an example Implementation
- Discuss an example Measurement
Course Content
ELECTRONIC HEALTH CARE (EHR) LIFE CYCLE
-
The author will discuss the EHR Life Cycle model: need, solution, implementation, and measurement; while lending thought to concepts integrated throughout the process: interoperability, stakeholders, hardware and software requirements, planning, execution, management, measuring effectiveness, and quality assurance.
-
Additionally, the author will discuss these concepts throughout an example of a hardware solution.
EHR LIFE CYCLE MODEL
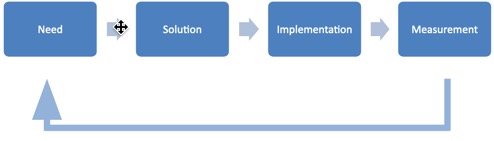
Need is accomplished by assessment of current functionality and business needs and identifying gaps and improvement opportunities. Solutions evolve from defining needs and opportunities, vendor review, design, and development. Implementation moves the process from testing to production, involves training, and support participation. Measurement evaluates full scale operation and yields direction for modification (Dimick, 2009).
THE NEED
Mission XYZ Hospital COO directive
-
Increase interdepartmental throughput between admitting, laboratory, pharmacy, and clinicians
-
Maintain existing software
NOTE: The McKinsey Global Institute found that 91 billion of health cares’ spending in the United States was spent due to inefficient and redundant health administration practices (Bentley, 2008).
Mission XYZ Hospital has evaluated the current systems and identified gaps in the process with room for improvement.
-
Best of breed platforms in place
-
Lack of Interoperability
-
De-centralized data exchange
-
Resulting delays in patient information and care
-
Readiness to industry standards
-
Delayed access to patient data
-
Duplicate data entry
-
Complicated downtimes
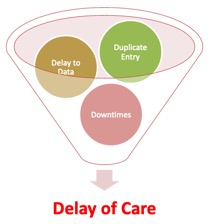
-
Stakeholders
-
Patients
-
Clinicians
-
Admissions
-
Laboratory Services
-
Pharmaceutical Services
-
Many are affected by the gaps identified. Patients, clinicians, admitting, laboratory services, and pharmaceutical services experiences duplicate data entry, delayed access to patient data, and complicated down times when one point in the system goes down or need updating are all typical problems straining efficiency of the health care data flow.
THE SOLUTION
-
Proposal for HL7 Integration Engine
-
Maintain current best of breed platforms
-
Replaces current point to point design with centralized data processing.
NOTE: Uniform coding of data is accomplished by HL7 as it was developed as a standard language for the sharing and integration of health data (Intersystems, 2013). It is reliable and reduces issues with interoperability among applications and facilities nationally and internationally.
- Yields
- Improved thought
- Less complicated maintenance
- Improved scalability
- Long term financial savings
- Planning
- Design | Requirements | RFP | Awareness
- Training | Support | Milestones | Costs
NOTE: Strategic planning should involve all stakeholders to ensure a thorough and successful process of defining, planning, implementation, communication, and controlling. Identifying a design that accomplishes the most bang for the buck, the RFP process, and setting expectations for training involve thorough assessment of business needs and developing functional requirement for vendors.
SOLUTION DESIGN
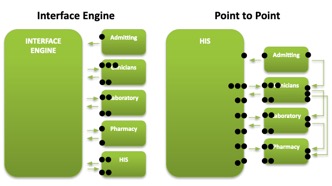
The solution will reduce the required number of export and import endpoints, allow for the reuse of data between applications, provide and easier method to interface a new or replaced application, provide the ability to monitor the entire system at one time, and provide the ability to proactively notify interested parties using visual alerts and emails when problems arise (Corepoint Health, 2010).
SOLUTION IMPLEMENTATION PLAN
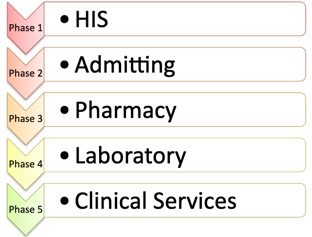
NOTE: The phased project will replace the current “home grown” design (Someshwar, 2013) with a central data processing model, allowing improved data flow, centralized maintenance, and scalability (Corepoint Health, 2010).
SOLUTION RFP

NOTE: Current hardware and software should be analyzed to prepare requirements for proposed solution. The request for proposal (RFP) process involves preparing a legal document presenting the need in detail for vendors to develop a solution. Costs are estimated for solution implementation, training, maintenance, future expansion, etc.
IMPLEMENTATION
Information exchange in health care information technology adoption faces technical barriers, economic barriers, and commercial barriers (HealthIT.gov, n.d.). Interoperability and lack of local/national infrastructure are expensive barriers to overcome.

Implementation takes the product into use and should involve prior testing. Awareness to all involved should take place prior to training and throughout the process.

Support is important to have in place from all key stakeholders including IT, upper management, and key departments. Change can be difficult and always involves user acceptance and often resistance. Success can be correlated to managing culture change.
IT resources should be in place not only for support but also ensuring continual security measures avoiding any breaches in privacy. Disaster planning should be accounted for a new implementation.
MEASURING
-
Measuring effectiveness
-
Quality assurance against goals and objectives
-
Controlling project focus
-
Training efforts
-
Root/Cause Analysis
-
NOTE: Measuring against defined goals and objectives is the last part of the process. It gives opportunity to control the project, training efforts, and perform root/cause in efforts to modify necessary items of implementation. This is a revolving process until all functionality and goals have been met.
STANDARDS
-
Standards
-
Management support
Management should support the push for standards. The Office of the National Coordinator for Health Information Technology (ONC) Comments on Patient Safety and Electronic Health Record Systems recommend the continual improvement of Information Technology (IT) to increase patient safety with emphasis on learning, improving, and leading (HealthIT.gov, 2013). We should seek to get federal and state legislation involved to help create mandates and standards that encourage interoperability. Without standards, many vendors do not fully understand or acknowledge the need to create software that allows interoperability. Healthcare providers may understand the need for interoperability but may cut corners to cut cost if standards are not set to promote interoperability.
REFERENCES
Bentley, T. (2008). Waste in the u.s. health care system: A conceptual framework. The Milbank Quarterly, 86(4), 629-659. doi: 10.1111/j.1468-0009.2008.00537.x
Corepoint Health. (2010). Why Do I Need an Interface Engine? [White paper]. Retrieved from http://www.corepointhealth.com/sites/default/files/whitepapers/why-healthcare-interface-engine.pdf
Dimick, C. (2009). Core Services to Support the EHR Lifecycle. Retrieved from http://journal.ahima.org/2009/06/16/core-services-to-support-the-ehr-lifecycle/
HealthIT.gov (n.d.). How does the HITECH Act address barriers to information exchange? Retrieved from http://www.healthit.gov/policy-researchers-implementers/faqs/how-does-hitech-act-address-barriers-information-exchange
HealthIT.gov (2013). Comments on Patient Safety and Electronic Health Record Systems Retrieved from http://www.healthit.gov/sites/default/files/hitpc_cawg_patient_ safety_hit_final.pdf
HIMSS. (2013). What is Interoperability? Retrieved from https://www.himss.org/library/ interoperability-standards/what-is
Intersystems (2013). HL7 Messaging with Ensemble. Retreived from http://www.intersystems.com/ our-products/ensemble/hl7-messaging/
Someshwar, P. (2013). Interoperability: Not a non-issue. Retrieved from http://www.healthcareitnews.com/blog/interoperability-not-non-issue
Course Exam
Before you receive your certificate, you must complete the exam and achieve a score of % or higher. (You have unlimted attempts).
This exam is required by your state licensure.
Exam
Exam
We are required to delay the exam hours. Check back soon!
Exam
We are required to delay the exam until you have had time to view the course material. Please view the course first!
No Licenses on File
Please add a license to your account before you continue. Thank you!
