Infection Prevention and Control in Long Term Care Part 2
Infection Prevention and Control in Long Term Care Part 2
Course Description
Infection Prevention and Control in Long Term Care is discussed including sypmtoms of pneumonia, UTI, C-diff, and the differences in CAI and HAI.
Accreditation Information: KLA Education Services LLC is accredited by the State of California Board of Registered Nursing, Provider # CEP16145.
Course Certification: Once you have completed this course, click on the “Print Certificate” option below to save or print your CE course certification. If you are not yet registered in a course plan with IvyLeagueNurse, please complete the registration and payment process so that you are able to log into your account and fully obtain your course certificate. Our affordable and unlimited one-year CEU plan starts at just $19.99.
Print Certificate Print Course
Course Objectives
Upon completion of this course, the course participant will be able to:
- List 3 signs and symptoms of pneumonia
- List 3 signs and symptoms of a UTI
- List 2 signs and symptoms of C-diff
- Describe the difference in CAI and HAI
Course Content
McGeer’s
-
Originally developed in 1991 to standardize the definitions of infection in the long-term care setting.
-
Revised in 2012.
-
Standard of practice in long-term care.
Surveillance Criteria
What it is...
-
For Surveillance only
-
Highly specific
-
Applied retrospectively
-
Focus on transmissible and preventable infections
-
Standardized
What it is NOT...
-
NOT for diagnostic purposes
-
NOT for clinical decision making
-
NOT for case findings
-
NOT based on a physician’s diagnosis only
-
NOT based on a single piece of evidence
McGeer’s Constitutionals
Fever
-
Any one of these findings:
-
A single oral temp of >37.8◦C (>100◦F) or
-
Repeated oral temp >37.2◦C (>99◦F) or rectal temp >37.5◦C (99.5◦F) or
-
>1.1◦C (2◦F) over baseline from a temp taken from any site
-
Leukocytosis
-
Either of these criteria:
-
Neutrophilia > 14,000 leukocytes/mm³ or
-
Left shift (>6% bands or >1500 bands/mmᵌ)
-
Altered Mental Status
-
All of the first 3 MUST be met and Either of the last two MUST be met:
-
Acute onset
-
Fluctuating course
-
Inattention
-
Disorganized thought
-
Altered level of consciousness
-
Functional Decline
-
A new 3 point increase in total ADL score from baseline based on 7 ADL items each scored from 0 - 4. The items are:
-
Bed mobility
-
Transfer
-
Locomotion in facility
-
Dressing
-
Toilet use
-
Personal hygiene
-
Eating
-
Respiratory Tract Infections
Common Cold
-
Must have at least two of the following:
-
Runny nose or Sneezing
-
Stuffy nose (congestion)
-
Sore throat, hoarseness or difficulty swallowing
-
Dry cough
-
Swollen or tender neck glands
-
Influenza-Like Illness (ILI)
-
Both criteria present:
-
Fever and Meet three of the following:
-
Chills
-
Headache or eye pain
-
Myalgias or body aches
-
Malaise or anorexia
-
Sore throat
-
Dry cough
-
-
ILI Change in Surveillance
-
Removed stipulation that diagnosis can only be made during the flu season
-
Now, can be diagnosed year round in accordance with CDC stan
Pneumonia
All of the Following Criteria:
-
CXR positive for pneumonia or a new infiltrate
-
One of the following:
-
New/increased cough
-
New/increased sputum
-
O2 sat< 94% on room air or reduce 3% from baseline
-
New/changed lung exam abnormalities
-
Pleuritic chest pain
-
RR >/= 25/min
-
AND...
-
One or more Constitutionals
-
Fever
-
Leukocytosis
-
Altered Mental Status
-
Functional Decline
-
Lower Respiratory Infection
ALL of the Following Criteria:
-
CXR not done or, negative for pneumonia or new infiltrate.
-
At least two respiratory S/S:
-
New/increased cough
-
New/increased sputum
-
O2 sat< 94% on room air or reduce 3% from baseline
-
New/changed lung exam abnormalities
-
Pleuritic chest pain
-
RR >/= 25/min
-
AND...
-
One or more Constitutionals
-
Fever
-
Leukocytosis
-
Altered Mental Status
-
Functional Decline
-
Pneumonia and LRTI
The presence of underlying conditions which could mimic a respiratory tract infection presentation, (e.g. CHF or interstitial lung diseases), should be excluded by a review of clinical records and an assessment of presenting S/S.
UTI (No Catheter)
Any One of the Following:
-
Acute dysuria or acute pain, swelling, or tenderness of the testes, epididymis, or prostate
-
Fever or leukocytosis AND...
One of the following:
- Costovertebral angle pain or tenderness
- Suprapubic pain
- Gross hematuria
- New/marked increase in incontinence
- New/marked increase in urgency
- New/marked increase in frequency
If NO Fever or Leukocytosis
-
At least two or more of the following:
-
Suprapubic pain
-
Gross hematuria
-
New/marked increase in incontinence
-
New/marked increase in urgency
-
New/marked increase in frequency
-
One of the Following:
-
>10⁵ cfu/ml of no more than 2 species of microorganisms in a voided urine or
-
> 10₂ cfu/ml of any number of organisms in a specimen collected by in and out catheter.
UTI Summarized:
- UTI = localized S/S & urine culture positive
Pyuria
-
Up to 90% of the elderly have pyuria all the time, so no need to treat for UTI just because of WBC’s in the urine.
-
The absence of pyuria excludes a DX of UTI
-
50 – 60% of elderly are colonized with organisms like E. Coli.
-
Pyuria does NOT differentiate Sx UTI from asymptomatic bacteriuria (ASB)
UTI (Catheter)
Any One of the Following:
-
Fever, rigors or new onset hypotension, with no alternate site of infection.
-
Either acute change in mental status or acute functional decline with no alternate diagnosis and Leukocytosis.
-
New onset suprapubic pain or costovertebral angle pain or tenderness
-
Purulent discharge from around the catheter or acute pain, swelling, or tenderness of the testes, epididymis, or prostate.
AND...
-
Urinary catheter culture with > 10⁵ cfu/ml of any organism(s)
-
(Specimen should be obtained after catheter is changed if in place > 14 days)
Evidence
-
In the absence of a clear source, acute confusion in a resident with a catheter and a positive urine culture are often treated, but evidence suggests that most episodes are NOT from a urinary source.
-
Recent catheter trauma, catheter obstruction or new onset hematuria are useful localizing signs consistent with UTI, but not necessary for diagnosis.
Skin and Soft Tissue Infection
CELLULITIS
One of the following:
-
Pus present at the wound, skin or soft tissue site OR
-
New/increasing presence of at least four of the following:
-
One constitutional criteria:
-
Heat
-
Redness
-
Swelling
-
Pain/tenderness
-
Serous drainage
-
-
CONSTITUTIONALS
-
Fever
-
Leukocytosis
-
Altered Mental Status
-
Functional Decline
Wounds
-
Presence of organisms cultured from the surface (e.g. swab culture) of a wound is not sufficient evidence that the wound is infected.
-
For wound infections related to surgical procedures, use the CDC and NHSN surgical site infection criteria and report these infections back to the institution performing the original surgery. (http://www.cdc.gov/nhsn/TOC_PSCManual.html)
-
More than one resident with streptococcal skin infection from the same serogroup (e.g. A, B, C, and G) in a LTC facility may suggest an outbreak.
Scabies
Both of the Following:
-
Maculopapular and/or itching rash AND
-
One of the following:
-
Physician diagnosis
-
Laboratory confirmation (scraping or biopsy) or
-
Epidemiologic linkage to a case of scabies with laboratory confirmation
-
Considerations
-
Rule out non-infectious skin conditions (E.g. eczema, allergy, skin irritation)
-
Epidemiologic linkage to a case of scabies with laboratory confirmation. Consider if evidence of geographic proximity in the facility, temporal relationship to the onset of symptoms or evidence of common source of exposure.
Fungal Oral/Perioral
Oral Candidiasis
-
Both of the following:
-
Presence of raised white patches on inflamed mucosa, OR plaques on oral mucosa
-
A medical or dental provider diagnosis
-
Considerations
-
Mucocutaneous candida infections are due to co-morbid conditions or antibiotic use.
-
Non-candidal fungal infections are rare.
Fungal Skin Infections
Must have Both
-
Characteristic rash or lesions AND
-
Either a medical provider diagnosis or laboratory-confirmed smear, culture or biopsy
Fungal Rash
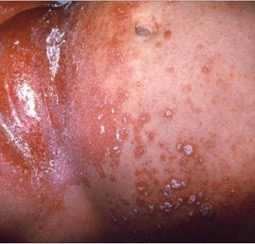
Herpes Viral Skin Infections
Must have Both
-
Vesicular rash
-
Either physician diagnosis or laboratory confirmation
Considerations
-
Reactivation of herpes simplex (cold sores) and herpes zoster (shingles) is not considered a HAI.
-
Primary herpes viral skin infections are very uncommon in a LTC facility.
Conjunctivitis
One of the following:
-
Pus from one or both eyes, present for at least 24 hrs
-
New/increased conjunctival erythema, with or without itching
-
New/increased conjunctival pain, present for at least 24 hours
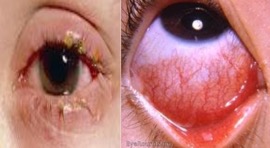
Considerations
- Conjunctivitis symptoms (“pink eye”) should not be due to allergic reaction or trauma.
Gastroenteritis
One of the following:
-
Three or > liquid /watery stools above resident baseline in 24 hrs
-
Two or > episodes of vomiting in 24 hrs OR
-
Both of these:
-
Stool specimen + for bacterial or viral pathogen AND
-
One of the following:
-
Nausea
-
Vomiting
-
Diarrhea
-
Abdominal pain/tenderness
-
-
Considerations
-
Exclude non-infectious causes of symptoms
-
New medications may cause diarrhea, nausea or vomiting
-
Initiation of new enteral feeding may be associated with diarrhea
-
Nausea or vomiting may be associated with gallbladder disease
Norovirus Gastroenteritis
Both criteria present
-
One of the following:
-
Diarrhea (three or > liquid/watery stools above resident baseline in 24 hrs) OR
-
Vomiting, two or > episodes in 24 hrs
-
-
Stool specimen + for norovirus by electron microscopy, enzyme immunoassay, or
-
molecular diagnostic test (PCR)
Outbreak Considerations
-
In an outbreak, confirm the cause
-
No confirmation, assume Dx by “Kaplan Criteria”
-
All criteria must be met:
-
-
Vomiting > 50% affected
-
Mean (median) incubation period 24-48 hrs
-
Mean (median) duration of illness 12-60 hrs
-
No bacterial pathogen cause identified
-
-
Clostridium Difficile
Both criteria present
-
One of the following:
-
Diarrhea (three or > liquid/watery stools above resident baseline in 24 hrs) OR
-
Presence of toxic megacolon by X-ray
-
-
One of the following:
-
Stool + for toxin A or B, or by molecular diagnostic test (PCR)
-
Pseudomembranous colitis identified during endoscopy, surgery, or in a biopsy
-
Considerations
-
Primary episode :
-
No prior episode OR
-
> 8 wks prior
-
-
Recurrent episode:
-
< 8 wks AND
-
Symptoms had resolved
-
-
Residents previously infected may remain colonized even after symptoms resolve
HAI if both criteria met
-
No evidence of incubation on admission
-
Based on documentation of S/S
-
Not just by screening microbiology data
-
-
Onset > two calendar days post admission
Considerations
-
Laboratory tests should only be done on diarrheal stool specimens unless ileus is suspected.
-
Repeat testing for the presence of C. Difficile toxins following treatment is not recommended.
More GI Considerations
-
Presence of new GI symptoms in a single resident may prompt enhanced surveillance for additional cases
-
In the presence of an outbreak, stool specimens should be sent to confirm the presence of norovirus, or other pathogens
-
In an outbreak, residents could test + for C. Difficile toxin due to ongoing colonization and also be co-infected with another pathogen AND
-
It is important that other surveillance criteria are used to differentiate infections in this situation
Blood Stream Infections
One of the following:
-
Two or > blood cultures + with same organism
-
Single blood culture + in the presence of:
-
Fever or hypothermia (< 34.5°C)
-
Drop in SBP of 30 mm/Hg from baseline
-
Altered mental status or functional decline
-
Considerations
-
Obtaining blood cultures is not recommended unless:
-
LTCF has quick access to laboratory facilities
-
Physician availability to respond rapidly to results AND
-
Capacity to administer parenteral antibiotics
-
Yours or Mine?
-
Community-associated Infection (CAI)
-
Healthcare-associated Infection (aka “Nosocomial) (HAI)
CAI vs. HAI
Community (CAI)
-
When clinical signs or symptoms are present on admission or
-
Manifest < 2 calendar days after admission
Healthcare (HAI)
- When clinical signs or symptoms of an infection are present AFTER the resident has been in the center > than 2 calendar days.
Infection vs. Colonization
Infection
-
Presence of clinical signs & symptoms
-
Organism growth & invasion of host
-
Presence of pathogen on a culture
Colonization
-
Absence of clinical signs and symptoms
-
No organism tissue invasion
-
Presence of pathogen on culture
Case Study # 1 “JH”
Answer = YES
- Fever - NO
- Altered Mental Status - YES
- Functional Decline - NO
- Leukocytosis - NO
- Respiratory Tract - NO
- Urinary Tract - YES (pain, 100,000 CFU/ml bacterial count)
Case Study # 2 “EH”
Answer = YES
- Fever - NO
- Altered Mental Status - YES
- Functional Decline - NO
- Leukocytosis - NO
- Respiratory Tract - NO
- Urinary Tract - YES (altered mental status, 100,000 CFU/ml MRSA)
Case Study # 3 “RP”
Answer = NO
- Fever - NO
- Altered Mental Status - NO
- Functional Decline - NO
- Leukocytosis - NO
- Respiratory Tract - NO
- Urinary Tract - NO
- GI Tract - NO
Case Study #4 "MM"
Answer = NO
- Fever - NO
- Altered Mental Status - NO
- Functional Decline - NO
- Leukocytosis - NO
- Respiratory Tract - NO
Case Study #5 "LH11"
Answer = NO
- Fever - NO
- Altered Mental Status - NO
- Functional Decline - NO
- Leukocytosis - NO
- Urinary Tract - NO
Case Study #6 "VV"
Answer = NO
- Fever - NO
- Altered Mental Status - NO
- Functional Decline - NO
- Leukocytosis - NO
- CXR - Progressive Infiltrate
- Respiratory Tract - New or increased cough productive
Case Study #7 "AN"
Answer = NO
- Fever - NO
- Altered Mental Status - NO
- Functional Decline - NO
- Leukocytosis - NO
- Urinary Tract - NO
Course Description
Course Objectives
Course Content
- McGeer’s
- Surveillance Criteria
- McGeer’s Constitutionals
- Respiratory Tract Infections
- ILI Change in Surveillance
- Pneumonia
- Lower Respiratory Infection
- Pneumonia and LRTI
- UTI (No Catheter)
- Pyuria
- UTI (Catheter)
- Evidence
- Skin and Soft Tissue Infection
- Wounds
- Scabies
- Fungal Oral/Perioral
- Fungal Skin Infections
- Herpes Viral Skin Infections
- Conjunctivitis
- Gastroenteritis
- Norovirus Gastroenteritis
- Clostridium Difficile
- More GI Considerations
- Blood Stream Infections
- Yours or Mine?
- CAI vs. HAI
- Infection vs. Colonization
- Case Study # 1 “JH”
- Case Study # 2 “EH”
- Case Study # 3 “RP”
- Case Study #4 "MM"
- Case Study #5 "LH11"
- Case Study #6 "VV"
- Case Study #7 "AN"
Course Exam
Before you receive your certificate, you must complete the exam and achieve a score of % or higher. (You have unlimted attempts).
This exam is required by your state licensure.
Exam
Exam
We are required to delay the exam hours. Check back soon!
Exam
We are required to delay the exam until you have had time to view the course material. Please view the course first!
No Licenses on File
Please add a license to your account before you continue. Thank you!
